Is cutting back on salt outdated advice? 🧠
Why the science looks messy - and what matters for your health
Advice about salt can feel confusing.
We’re told to cut back because of links with blood pressure and heart disease.
Yet you’ll also hear claims that this advice is outdated, and that eating too little salt could be harmful.
Add in studies that seem to point in different directions, and it’s no wonder people feel unsure.
So does how much salt you eat actually matter?
What we’ll cover today:
Why we keep arguing about salt
How some studies get misread
Where potassium helps - and where it doesn’t
How to think about salt day to day
Salt vs. sodium
Salt comes from underground deposits or from seawater that’s evaporated to leave salt crystals behind.
What we know as table salt, is actually sodium chloride, a compound made up of sodium and chloride.
Sodium helps regulate fluid balance and allows nerves and muscles to work properly. Chloride also supports fluid balance and is needed to make stomach acid for digestion. Both are essential, but it’s the sodium part of salt that’s most closely linked to blood pressure.
That’s why advice focuses on how much salt we eat overall. In the UK, it’s recommended to eat no more than about 6g a day of salt (around 1 level teaspoon, equal to about 2400mg of sodium). That includes the salt already present in food, as well as the salt we add in cooking.
On average though, we’re eating over this - closer to 8–9g a day.
Most of the sodium we eat comes from everyday foods like bread, cheese, cereals, sauces and ready meals, rather than what we add when cooking at home. Sodium is also found naturally in fruit and vegetables, but usually in very small amounts.
Salt and blood pressure
When we eat too much sodium, the body keeps more water, which increases the pressure inside blood vessels. Over time, this puts extra strain on the heart and circulatory system.
That’s why raised blood pressure is one of the strongest risk factors for heart disease and stroke.
It’s especially dangerous because many people don’t realise they have blood pressure problems until it’s picked up during a routine check, and why it’s often called a silent killer.
In the US, heart and circulatory disease is the leading cause of death, and the second main cause of death in the UK.
That’s why salt is taken seriously in public health advice.
In people with high blood pressure, salt reduction has a clear and meaningful effect. In people with normal blood pressure, the average drop is smaller, but it still moves in the right direction.
Some people are more sensitive to salt than others because of factors like age, genetics or existing blood pressure. Around one in three healthy adults are classed as salt sensitive, rising to over half of people with high blood pressure, and it becomes more common as we get older. But it isn’t an on–off switch. Even people who aren’t labelled salt sensitive usually still see their blood pressure go up, but less dramatically, when eating too much salt.
The J-curve confusion
You may have heard that too little sodium is also bad for your health.
That idea mainly comes from a few large population studies, like the PURE study. These types of studies don’t change what people eat, instead they look for patterns in large groups of people, like the links between estimated sodium and risk factors or disease.
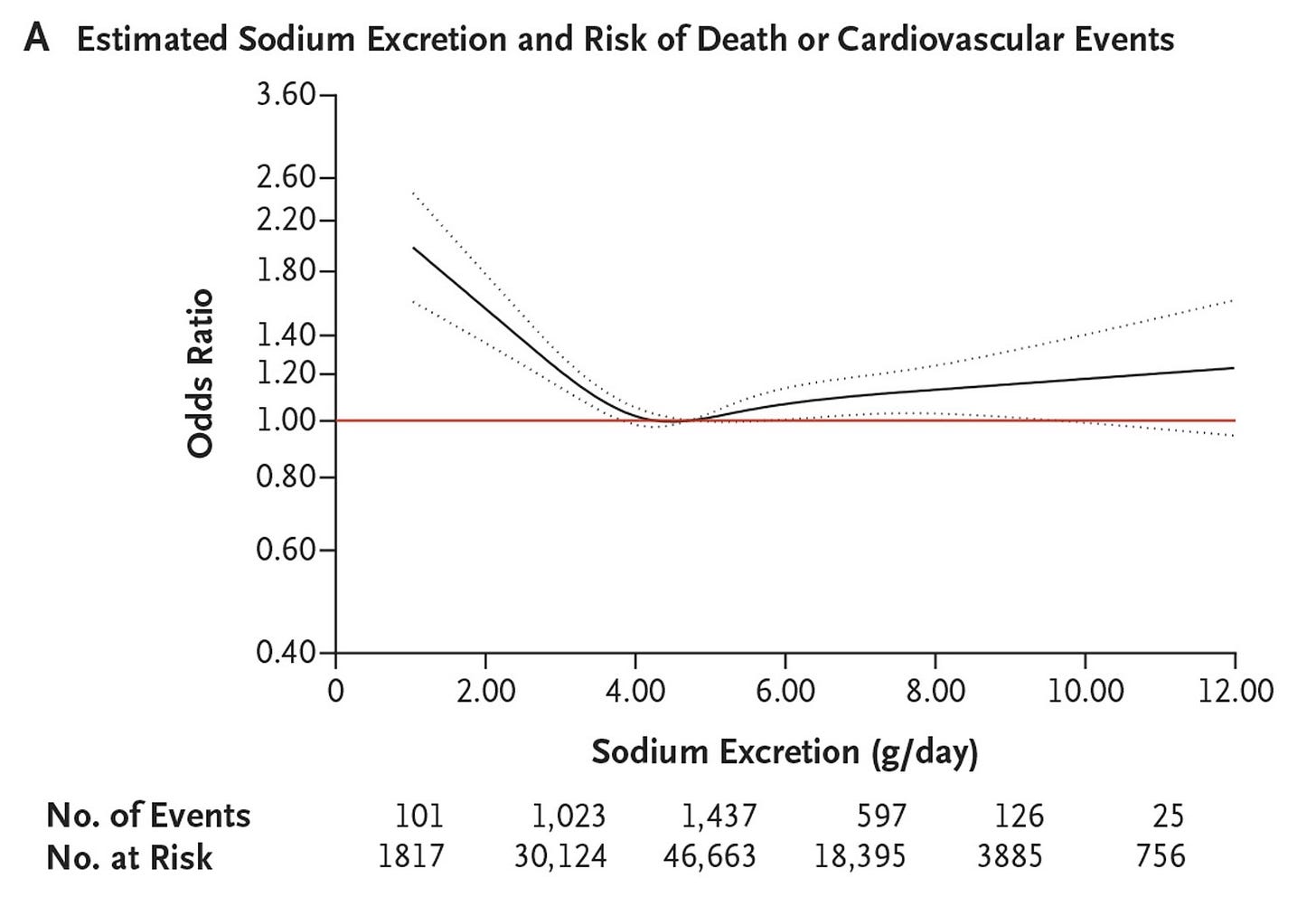
In the PURE study, they found that people who ate a lot of sodium were more at risk, mainly in people with high blood pressure. But the risk also appeared to be higher for the people who were estimated to have eaten the least sodium, too. When you plot that on a graph, it forms a J shape - with risk rising at both ends.
That can sound worrying. But there are two main reasons this pattern can be misleading:
Sodium wasn’t measured directly.
Many population studies estimate sodium from a single spot urine sample because it’s easier than a full 24-hour collection. But sodium levels change a lot during the day, so people can easily be misclassified - especially at the low end.Reverse causation
People who are unwell, tend to eat less and be advised to cut back on sodium, and are then more likely to fall into the lower sodium group. That can make lower sodium look risky, even when it isn’t the cause.
What about the rise in stress hormones you sometimes hear about?
There’s a worry that cutting salt may push up your stress hormones. When salt is cut suddenly, your body can briefly switch on hormones like adrenaline and noradrenaline to keep blood volume and blood pressure stable. That response is normal and protective, similar to what happens with dehydration or standing up quickly. And it settles.
In longer studies of four weeks or more, including studies where sodium was dropped to around or below 2000mg a day (<5g salt), those hormones, cholesterol and kidney markers looked no different, while blood pressure is lower.
Intervention studies often matter more
Population studies can spot patterns, but they can’t tell us what’s causing what.
Intervention studies are clearer - researchers deliberately change how much sodium people eat and are able to closely track to see what happens.
In the DASH–Sodium trial, adults with and without high blood pressure were assigned one of two diets, then randomly cycled through high, medium and low levels of sodium, down to about 1,500mg of sodium a day (about 2/3 teaspoon of salt). Sodium was checked using 24-hour urine collections.
As sodium went down, blood pressure went down too, in people with and without high blood pressure, with the biggest drop at the lowest sodium level. Stepwise, and no J-curve.
That’s why well-run trials often carry more weight than patterns from population studies.
Potassium and sodium: why balance matters
Potassium is another electrolyte, but it works differently from sodium. It can help the body get rid of excess sodium through the kidneys and relax blood vessels. While it doesn’t cancel out sodium, it softens some of sodium’s effects on blood pressure.